You were standing in the kitchen when you saw the video, so you put down your phone and kicked off your shoes to try it. You stood near the counter, just in case, and lifted one leg, only to feel your ankle wobble and your foot hit the floor before you even hit the five-second mark.
You didn’t say it out loud, but that quiet flicker of dread settled in: If I can’t even stand still for ten seconds, is my body already failing in ways I can’t fix?
At this age, every physical limitation feels like a permanent verdict rather than a starting point, especially when a simple balance test is being linked to how long you might live. But here is the truth: The one-leg balance test isn’t a “death sentence” or a sign that you are suddenly fragile. It is a vital check-up for a specific system in your body that most of us simply stop using after 40.
David noticed his confidence on morning walks shifting after he struggled with this exact test. That is his experience, not a set timeline for everyone. How your body responds depends on your current activity level, your inner ear health, and factors neither of you can fully control.
This article explains what the research shows and does not replace a clinical diagnosis. Before taking any step described in this article, consult a qualified healthcare provider. What applies generally may not apply to your situation, and acting without professional guidance here carries real risk.
What the 10-Second Test Actually Measures
If you can’t stand on one leg for 10 seconds after 50, it means your brain and muscles are struggling to communicate in real-time to keep you upright. It measures your “postural stability,” which is your body’s ability to sense a wobble and correct it before you fall.
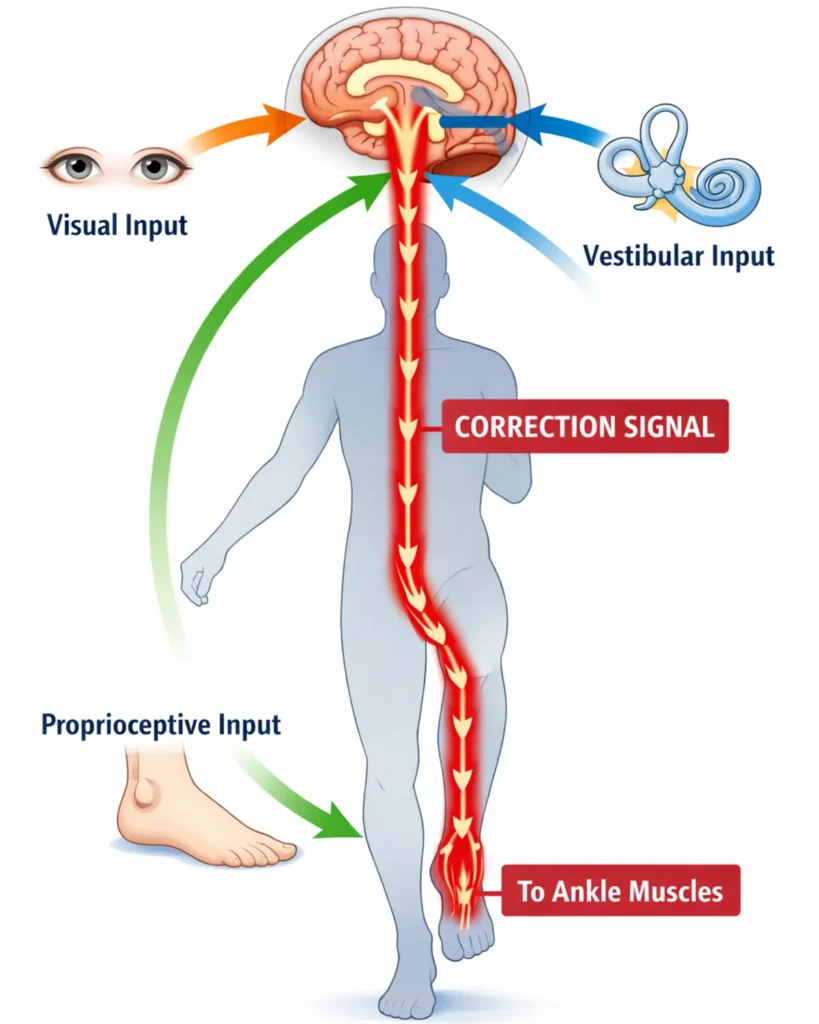
While it feels like a simple test of leg strength, it is actually a high-speed data check for your nervous system. To stay on one foot, your brain must constantly process signals from your eyes, your inner ears, and the nerve endings in your feet. If any part of that “conversation” is lagging, you lose your balance.
Researchers use this 10-second window because it is the tipping point where age-related decline usually shows up. For most adults, being unable to hit this mark isn’t about one specific disease; it is a “red flag” that your overall physical coordination is dipping below the safety zone.
You’re doing this right if you can keep your foot off the ground for the full count without grabbing a support, even if your standing ankle is shifting slightly to keep you centered. That small shifting is actually a sign of a healthy, responsive system.
But even if you passed, that doesn’t explain why this specific skill seems to vanish the moment we hit our fifties.
Why Balance Gets Harder After 50
Balance is a “use it or lose it” skill that relies on a mechanism called proprioception [the body’s ability to sense its own position in space without looking]. Think of it like a GPS for your limbs; it tells your brain where your feet are even when your eyes are closed.
As we age, the sensors in our joints and muscles become less sensitive. At the same time, we often stop doing the movements that keep these sensors sharp, like hiking on uneven ground or playing sports. When you stop challenging your proprioception, the “GPS signal” gets weak and fuzzy.
The second factor is your vestibular system [the tiny, fluid-filled tubes in your inner ear that detect motion]. This system acts like a carpenter’s level for your head. After 50, the fluid and tiny “stones” in these tubes can become less responsive, leading to that “wobbly” feeling when you turn your head quickly or try to stand on one foot.
What David noticed was that he had stopped moving in ways that challenged these systems. He walked on flat pavement and sat in sturdy chairs. His brain wasn’t “broken”; it was just out of practice. What worked in his case won’t be identical to yours, but the underlying pattern of “sensory rust” is common for almost everyone.
This “rust” isn’t just an inconvenience. It’s the reason why researchers are so interested in your balance as a predictor of your future health.
What the Research Says About Your Risk
A major 2022 study in the British Journal of Sports Medicine followed 1,702 adults aged 51 to 75 for seven years.
Those who couldn’t complete the 10-second stand had a significantly higher risk of all-cause mortality, meaning death from any cause, within the following decade
Specifically, the risk was nearly double for those who failed compared to those who passed. This sounds terrifying, but it is important to understand why the numbers look this way. Balance isn’t just about falling; it is a proxy for your “biological age.”
If you have good balance, it usually means you have:
- Better cardiovascular health (blood is reaching your brain and nerves efficiently)
- Higher muscle mass (which protects your metabolism)
- Better cognitive function (your brain’s processing speed is high)

In other words, your balance score is a window into systems your doctor might not think to test until something goes wrong.
David’s inability to hold the test was one of those first visible signals. He had no diagnosed condition, but his body was flagging something worth paying attention to. What showed up in his case won’t mirror yours exactly, but the pattern the research identifies is consistent.
Yet, as alarming as the “double risk” stat sounds, it doesn’t mean your clock is ticking down to zero.
What Failing Doesn’t Mean (This Matters)
Failing this test today is not a diagnosis of a terminal illness. It is a data point, not a destiny. Many people fail the test simply because they are wearing the wrong shoes, have a temporary inner ear flare-up, or haven’t practiced a balance-based movement in twenty years.
Doctors use several balance assessments depending on the setting. The 4-Stage Balance Test (standing with feet in progressively narrower positions), the Timed Up and Go (standing from a chair, walking 10 feet, and returning), and the Berg Balance Scale (14 different movements scored) are all common clinical tools.
10-second one-leg stand is the one most studied for longevity because it’s simple, requires no equipment, and predicts long-term outcomes with surprising accuracy.
It’s easy to look at a “failed” test and feel like your body is declining faster than your peers. But unlike your height or your genetic history, balance is highly “plastic.” This means your brain and muscles can actually rebuild the connections needed to stay upright at any age.

If you failed today, it likely means you’ve been living in a “flat-surface world” where your balance systems haven’t been challenged. It is a sign to start training, not a reason to start panicking. The real danger isn’t the 10-second failure itself; it’s the choice to ignore the signal and do nothing about it.
The real shift shows up not in the test itself, but in the small daily drills you do afterward.
How to Start Building Balance Back
The goal isn’t to become a circus performer; it’s to sharpen that internal GPS signal so your body feels “locked in” during daily life. You can improve balance over 50 by incorporating “micro-challenges” into your day.
Start with your hand on the counter. If you cannot hold 5 seconds even with support, or if you feel dizzy, stop and see a physical therapist before continuing.
The “Brush and Balance” Protocol The easiest way to start is by using an existing habit. When you brush your teeth tonight, try to stand on one leg for as long as you can.
- The Position: Keep your standing knee slightly “soft” (not locked).
- The Action: Lift your other foot just two inches off the floor. Keep one hand hovering near the sink for safety.
- The Duration: Aim for 30 seconds total per leg, even if you have to put your foot down several times.
- What to Notice: You are doing this right if you feel the small muscles in your feet and ankles “firing” or twitching. That twitching is your nervous system recalibrating in real-time.
The “Three-Point” Touch If standing on one leg feels impossible right now, start with your toe touching the ground for balance. Gradually reduce the pressure on that toe until you are lifting it for one second, then two.
David started with the “sink-side” method, holding on with just one finger before eventually letting go entirely. His experience is one example, but the principle of “progressive challenge” applies to everyone.
The frustrating part is that your brain gets better at balance before your body gives you any obvious proof that it’s working.
How Long Before You See Real Results?
You will likely notice a change in your “steadiness” long before you see a change in your muscle size. This is because balance improvements happen in the nervous system first.
Within two to three weeks of daily practice, your brain becomes more efficient at filtering the “noise” from your inner ear and focusing on the signals from your feet. You might notice that you don’t stumble as often when stepping off a curb, or that you feel more confident walking on a rug or grass.
The “10-second” mark is a great baseline, but the real victory is the “functional” balance you gain: the kind that keeps you active and independent for the next thirty years.
Your Questions Answered
Why can’t I balance on one leg anymore?
Most people lose this ability because of a decline in proprioception: your body’s internal sense of where its limbs are. When we stop performing varied movements like climbing or balancing, the nerve pathways between the feet and brain become “rusty” and slow to react.
Is the 10-second balance test accurate?
Yes, as a general screening tool for biological age and mortality risk in adults over 50. While it cannot diagnose a specific disease, research shows it is a reliable indicator of overall physical “frailty” and long-term health outcomes.
Can you improve balance after 50?
Absolutely. Balance is a motor skill, similar to typing or riding a bike. Daily stability drills give your brain the signal it needs to create new neural pathways and strengthen the stabilizer muscles in your ankles and hips.
What causes balance loss with age?
The most common causes are a combination of muscle loss (sarcopenia), reduced sensitivity in the inner ear (vestibular system), and slower nerve conduction. However, many of these factors can be slowed or partially reversed with targeted exercise and balance training.
How long should I be able to stand on one leg for my age?
Research shows average hold times: age 50-59: 37 seconds, age 60-69: 30 seconds, age 70-79: 18-22 seconds, age 80+: 10-15 seconds. The 10-second test is a minimum threshold, not the goal. If you’re hitting these averages, your balance is on track.
Conclusion
Struggling with the one-leg balance test is a wake-up call, but it’s one you are fully capable of answering. This simple movement is the ultimate “check-engine light” for your body’s internal navigation system. Balance is a skill you maintain, and that single shift in how you see it changes what you do about it tonight.
Start tonight at the bathroom sink. Don’t worry about the 10-second clock yet. Just worry about feeling the floor beneath your feet and the “wobble” that means your brain is learning again.
Your Balance Protocol:
- The Sink Test: Attempt the one-leg stand while brushing your teeth to find your baseline.
- The “Soft Knee” Rule: Never lock your standing leg; keep it slightly bent to engage your muscles.
- The 3-Week Drill: Practice for 30 seconds per leg every single day.
You aren’t just “standing on one leg.” You are retraining your brain to keep you steady for the decades ahead.
⚠️MEDICAL DISCLAIMER
This content is for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. Before making changes to your diet, exercise routine, or supplement regimen, consult a qualified healthcare provider. If you experience sudden, severe dizziness, chest pain, or joint pain during exercise, seek emergency medical care immediately.