You’re sitting on the sofa after dinner, but you can’t get comfortable. There is a dull, heavy pressure tucked right under your bottom rib on the right side. Then you feel it: that weird, aching radiation reaching up toward your right shoulder blade. It’s the signature that tells you this isn’t just “gas.”
That pressure after a slice of pizza? It isn’t in your head. For many people, the first real “warning shot” happens on a night exactly like this and it’s far more common than most doctors mention. For many, the first real “warning shot” happens on a night exactly like this.
If you’re thinking you have to give up every food you love just to stop the hurting, here is why this is different. Most advice focuses on a “fat ban.” But the real issue is often about how your body moves that fat through your system. You might feel like your body is failing you, but it’s likely just a mechanical bottleneck.
Gallbladder pain after eating fatty food is a signal that your “internal plumbing” needs a change in strategy, not a total shutdown. We are going to move from “damage control” to a protocol that restores flow.
Vera sits on her sofa, rubbing her side. She chose the grilled salmon tonight, a “healthy” choice, yet she feels the same heavy ache she got from last week’s pepperoni pizza. She worries her family history is finally catching up to her.
Gallbladder Pain After Eating Fatty Food: The Sludge Factor
It is not your fault that your digestion feels sluggish. As we age, our internal mechanics simply change. To stop this stagnation tonight, follow the Bile Flow Protocol:
- The 1-Tablespoon Boundary: Limit your fat intake to one level tablespoon per sitting during an active flare-up. This provides enough fat to signal a gentle contraction of the gallbladder without forcing a “hard squeeze.”
- The Bitter Trigger: Eat a small amount of bitter greens, like arugula or radicchio, a few minutes before your main meal. Bitter flavors stimulate the release of cholecystokinin (CCK — the hormone that signals your gallbladder to contract). This is the hormone that tells the gallbladder to wake up.
- The Post-Prandial Pivot: Stand up and walk at a slow, leisurely pace for ten minutes immediately after finishing your last bite. Gentle movement uses gravity and light abdominal shifts to help the stomach empty faster.
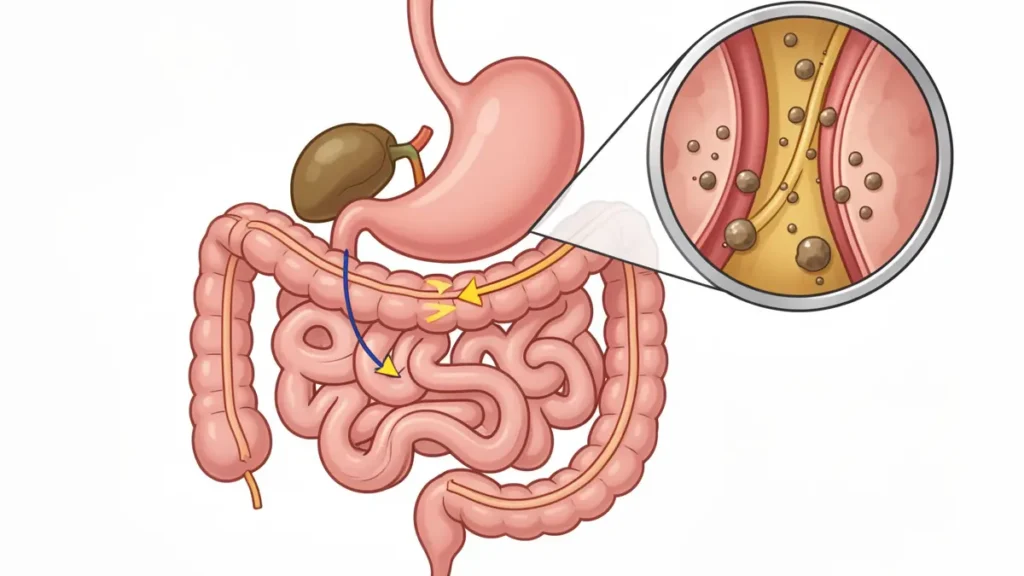
Your gallbladder acts like a rechargeable soap dispenser. It is a storage organ for bile. It waits for fat to enter the small intestine, then pumps out bile to break that fat down. If that “soap” sits too long without being pumped, it begins to thicken into a gritty “sludge” or hardens into stones.
Passing age 50 often brings hormonal shifts and a natural slowing of the digestive tract. This makes it easier for bile to stagnate. When you finally eat a fatty meal, the gallbladder tries to squeeze. But it’s trying to push thick “molasses” through a tiny straw. This creates the pressure you feel under your ribs.
What this means for you: your goal isn’t to avoid fat entirely , it’s to keep the bile moving in small, manageable waves so the pump never has to force it
Vera remembers her mother’s surgery. She fears her genes are the only factor here. While biology plays a role, shifting toward these movement-based habits helps manage the physical reality of how her bile flows.
No two gallbladders are the same. What works for one person may need adjusting for another.
Pain After Eating Fatty Food: Why the 2-Hour Window Matters
Gallbladder pain after eating fatty food typically begins 60 to 120 minutes after a meal. This occurs because the body releases CCK to signal the gallbladder to contract. If gallstones or thick bile (sludge) are present, the gallbladder squeezes against a blockage, creating internal pressure and pain.
This hormone acts like a “squeeze” command. If you have gallstones, the gallbladder tries to contract against a blockage. This creates a backup of pressure. It is much like a balloon being squeezed with the nozzle tied shut. What this means for you: the pain isn’t random, it follows a predictable 60-to-120-minute window you can plan around. This explains why the pain feels like a deep, internal pressure rather than a sharp skin-level sting.
To manage this “pressure window” effectively:
- Hydrate with Warmth: Sip 8 ounces of warm lemon water during your meal. Warm liquids help relax the smooth muscle of the digestive tract. Ice-cold drinks can cause minor spasms that make the “squeeze” feel more intense.
- The “Slow-Drip” Method: Portion your fats across the entire day. Smaller, frequent signals to the gallbladder keep the bile moving in small “puffs” rather than one massive contraction.
- The Posture Check: Sit upright for at least two hours after eating. Slumping on a deep sofa compresses the abdominal cavity. This can increase the mechanical pressure on the gallbladder area.
Vera noticed that her worst nights always followed a large, late-evening meal. Shifting her largest fat intake to earlier in the day made the heavy sensation under her ribs feel much lighter.
Gallbladder or Gas? The 30-Second Self-Check
Gallbladder pain after eating fatty food shares its address with two common impostors: trapped gas and a pulled muscle on your right side. Telling them apart changes everything about how you respond. The gallbladder has a very specific “address” in your body. Because the nerves serving the gallbladder also travel near the spine, the pain often “telegraphs” to strange locations.
Colin once thought he had simply thrown out his back. He spent time icing his right shoulder blade, assuming yard work had caught up to him. He only realized the source was internal when the ache intensified after a heavy breakfast.
How to Perform the 30-Second Self-Check:
Your body will respond in its own way. Treat this as a starting point, not a rulebook.
Common Mistakes: Why “Zero Fat” Actually Hardens Stones
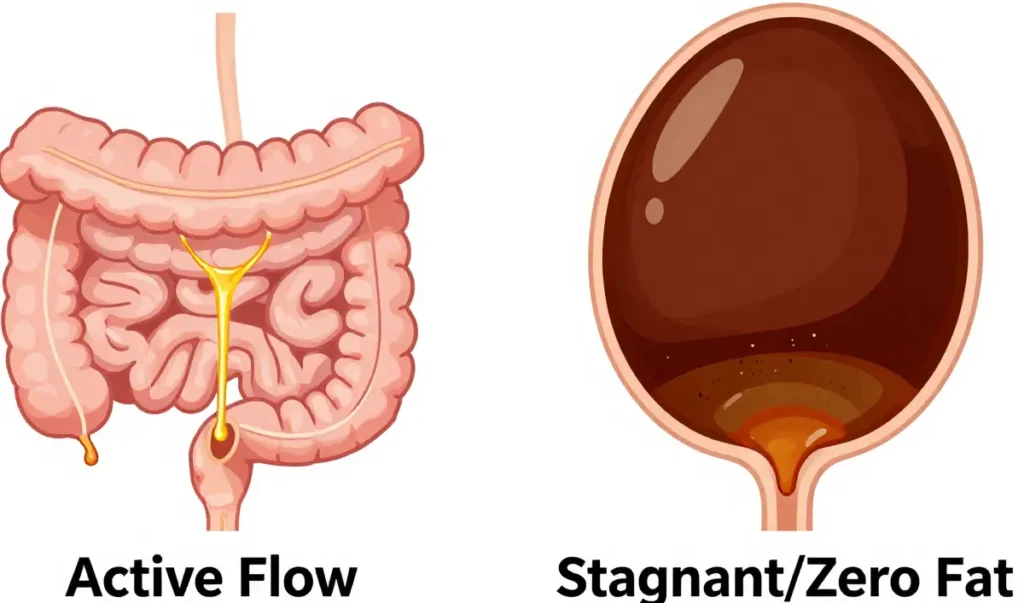
This is the part most guides skip: when the right side starts aching, the natural instinct is to cut out every gram of fat. You might think that “starving” the gallbladder gives it a rest. In reality, a zero-fat diet can make the problem worse.
Bile is a “use it or lose it” fluid. When you stop eating fat entirely, the gallbladder stops squeezing. The bile just sits there, becoming more concentrated. Over time, this stagnant pool is exactly what turns from thin liquid into thick “sludge.”
How to Avoid the Stagnation Trap:
- The 5-Gram Minimum: Ensure every meal contains at least 5 grams of healthy fat (about a teaspoon of olive oil). This is the “threshold” required to trigger a gentle contraction.
- Avoid “Invisible” Fats: Stick to whole-food fats. The hidden, processed fats in “low-fat” snack bars are often harder for the body to emulsify.
- The Fiber Buffer: Pair your small fat portion with soluble fiber, such as half a cup of cooked oats or a small pear. Fiber binds to old bile salts and carries them out of the body.
Vera had tried eating only plain white rice and steamed vegetables, yet the pain never truly vanished. She eventually found that adding a tiny drizzle of flaxseed oil to her morning bowl helped her feel less heavy by midday.
No two gallbladders are the same. What works for one person may need adjusting for another.
The “Bile Flow” Action Plan
You are the primary investigator of your own body, and you don’t need to live on steamed broccoli forever. The goal is to manage the concentration of your bile so it flows like water rather than sludge.
Colin found himself at a family BBQ. Instead of skipping the meal, he used the Emergency Safe Plate protocol. He took a small portion of lean meat and filled half his plate with vinegar-based coleslaw. He walked the perimeter of the yard while talking to his cousins. He found he could enjoy social eating without the dread of a midnight flare-up.
How to Build Your Plate Around Bile Flow
Your kitchen is the starting point. No appointments needed.
Start every meal with a bitter trigger. A small handful of arugula, a squeeze of lemon juice over your plate, or a few slices of radicchio stimulates CCK release before the fat arrives. Canned or frozen greens work just as well as fresh.
Keep fat to one level tablespoon per sitting during a flare. One teaspoon of olive oil drizzled over cooked oats counts. So does a quarter of an avocado mashed onto toast. That’s your threshold. Enough to prompt a gentle squeeze, not a hard one.

Pair every fat portion with soluble fiber. Half a cup of cooked oats, a small pear, or a cup of cooked lentils binds old bile salts and carries them out. Buy oats and lentils in bulk. They’re among the most affordable options in any grocery store.
Walk for ten minutes after your last bite. Slow and flat is fine. This isn’t exercise. It’s gravity-assisted digestion. A lap around the block or pacing your hallway both count.
Track two free metrics starting tonight. First, your pain window: note the time you finish eating and the time discomfort begins. Second, your fat portion: one tablespoon or less versus more. Patterns emerge quickly.
When your next doctor visit arrives, bring these two requests.
Request a right-upper-quadrant abdominal ultrasound if you have recurring pain after meals. This is the standard first-line test for gallstones and sludge.
Ask specifically for a fasting ultrasound. Eating beforehand can make the gallbladder contract and hide findings.
Request a basic liver panel alongside it. Elevated bilirubin or liver enzymes gives your doctor a fuller picture of bile flow.
If the ultrasound shows nothing but pain continues, one more test exists.
A gastroenterologist can order a HIDA scan. This nuclear imaging test measures how efficiently your gallbladder empties. A low ejection fraction points to functional gallbladder disease even without visible stones.
It’s optional. But it’s the clearest answer available.
Your body will respond in its own way. Treat this as a starting point, not a rulebook.
When “Wait and See” Becomes a Risk: The ER Checklist
While many gallbladder issues can be managed through flow management, there is a point where the bottleneck becomes a medical emergency. If a stone leaves the gallbladder and gets stuck, it can cause a dangerous backup.
Use this ER Checklist to see if your pain has crossed the line:
- The Fever Test: Rib pain accompanied by a fever over 101°F or shaking chills often indicates an infection.
- The Skin Check: Look in the mirror at the whites of your eyes. If they appear yellowish, or if your urine has turned the color of dark tea, bile is likely backing up.
- The Duration Rule: Typical gallbladder “attacks” subside within six hours. If you have unrelenting, agonizing pain for longer than this, seek help.
- The “Phantom” Relief: If intense pain suddenly vanishes but is replaced by a high fever, the gallbladder may have perforated.
Your Questions Answered
How do you calm gallbladder pain in the moment?
When pain has already started, stop eating immediately. Sit upright rather than slumping forward. Sipping warm water slowly helps relax the smooth muscle around the digestive tract while your body works through the contraction cycle.
What foods cause the worst gallbladder attacks?
Fried foods, full-fat dairy, and processed meats top the trigger list. These are high in saturated fat, which demands a strong gallbladder contraction to emulsify. Spicy foods and cruciferous vegetables like broccoli can also worsen bloating during a flare, though they aren’t fat-related triggers.
Q: Is gallbladder pain more common after 50?
Yes. Hormonal changes after menopause reduce bile acid cycling, making bile thicker and slower to move. Men over 50 also see an increase as metabolism slows and cholesterol balance shifts.
Conclusion
Managing gallbladder pain after eating fatty food is about moving away from the “fear of fat” and toward “flow management.” By understanding that your gallbladder is a pump that needs regular, gentle exercise, you can reduce that heavy pressure.
Tomorrow, I’m testing the “1 Tbsp + 10-Minute Walk” rule.
Vera’s hope returned when she realized she didn’t have to live on white toast. She began planning her lunch with fresh greens and a small drizzle of olive oil, followed by a quick stroll. Gradually, she noticed that the “balloon” feeling didn’t return. You have the resources to begin this shift today.
Your Gallbladder Protocol:
- Trigger: Start meals with a bitter flavor (lemon or greens).
- Limit: Keep fat to 1 tablespoon per sitting during flares.
- Flow: Walk for 10 minutes after dinner to assist digestion.