If your gums bleed when you brush, your heart may be paying the price. Most people grab a tissue, rinse, and move on. They assume it’s from brushing too hard. Or that it’s normal. It’s not. Almost 60% of adults over 65 have periodontal disease, and the majority have no idea it’s connected to heart risk. Your dentist mentions it. You nod. You leave. Nothing changes.
The same bacteria destroying your gum tissue can travel through your bloodstream and damage your arteries. This isn’t a fringe theory. Exactly how oral bacteria reach your heart. Why does your risk compound sharply after 50? Five steps you can take this week, no prescription needed.
What Is Gum Disease and Why Is It So Common After 50?
Gum disease is an infection. That’s the simplest way to put it. It starts as gingivitis, with red, swollen gums that bleed easily. At this stage, it’s reversible. Most people ignore it. Then it becomes periodontitis, in which the infection spreads below the gum line and begins destroying the bone that holds your teeth in place. That damage is permanent.
Bacteria build up in a sticky film called plaque along your gum line. If plaque isn’t removed daily, it hardens into tartar. Your immune system attacks the infection. In doing so, it also attacks the surrounding tissue and bone. Pockets form between your teeth and gums. Bacteria move deeper. The cycle continues quietly, painlessly, for months or years. That silence is the danger.

Most cases of periodontitis cause no pain until it’s advanced. A 57 year old notices her gums bleed when she flosses. She flosses less to avoid it. The pockets deepen. She doesn’t know anything is wrong until her dentist tells her she’s lost bone around four teeth. This story is extremely common. And after 50, the risk gets worse for several reasons.
Your immune response weakens with age. Bone density decreases throughout your body, including in your jaw. Many common medications for blood pressure, allergies, and depression cause dry mouth, which removes the saliva that naturally cleans your teeth. Add diabetes, smoking, or stress, and the conditions become almost perfect for gum disease to grow.
The Science: How Gum Disease Reaches Your Heart?
Every time you chew with infected gums, bacteria can enter your bloodstream. That’s the whole mechanism. A healthy gum forms a tight seal around each tooth. An infected gum pulls away and creates a pocket, an open wound, essentially, lining the inside of your mouth. Bacteria live in that pocket.
When you eat, brush, or even just clench your jaw, those bacteria squeeze into your blood. Once in your bloodstream, they travel. Researchers have found oral bacteria, specifically a species called Porphyromonas gingivalis, inside fatty arterial plaque far from the mouth.
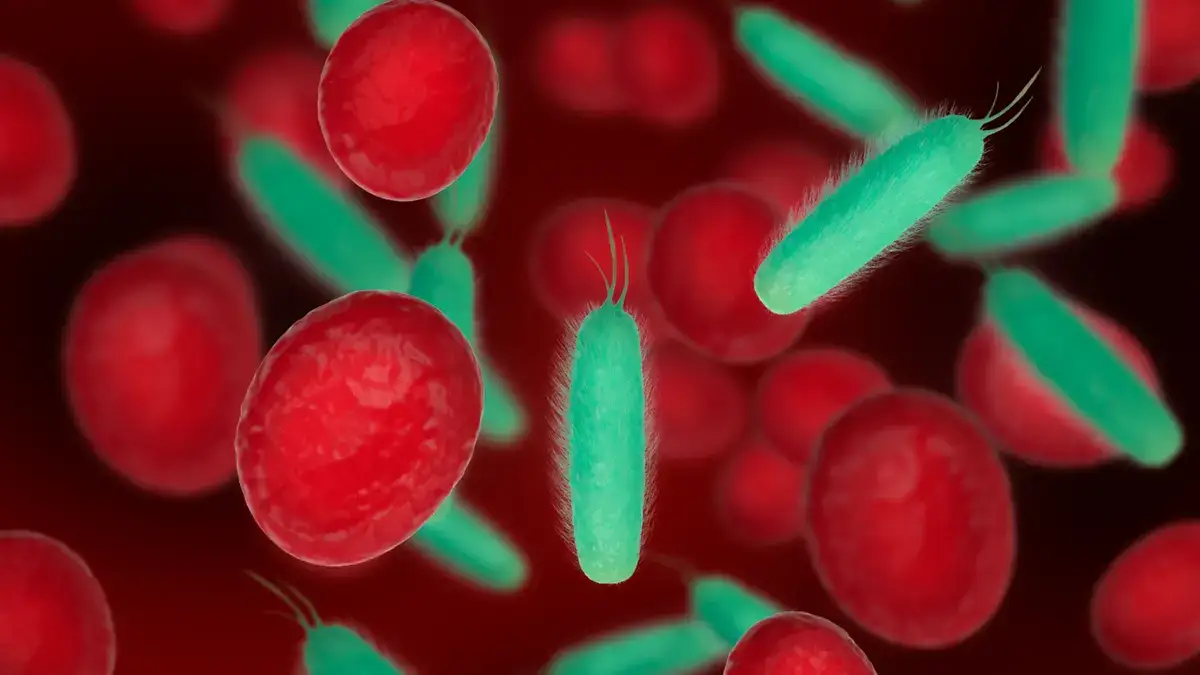
Not near the mouth. Inside clogged arteries in the heart. This isn’t a theory. It’s been confirmed through autopsy level analysis of arterial tissue.
Why People Over 50 Face a Compounded Risk?
After 50, two of the most common chronic diseases in the world collide. Gum disease peaks in prevalence between ages 50 and 75. Cardiovascular disease risk rises sharply in the same window. This isn’t a coincidence. The same conditions that fuel one tend to fuel the other.
Shared risk factors include type 2 diabetes, high blood pressure, smoking, obesity, and low physical activity. Each one increases both gum disease severity and heart disease risk. But they don’t just add the risks together; they amplify them. Take diabetes. People with severe periodontitis and type 2 diabetes have 3.2 times the mortality risk compared to those with no or mild gum disease.
The connection goes both ways: uncontrolled blood sugar worsens gum infections, and active gum infections make blood sugar harder to control. Add bone loss to the picture. Advanced periodontitis destroys the bone supporting your teeth. Tooth loss follows.
An Australian study of 172,630 adults with cardiovascular disease found that tooth loss independently predicts ischemic heart disease. A Netherlands study of 60,174 adults reached the same conclusion: clinical periodontitis had an independent link to atherosclerotic cardiovascular disease.
Many heart medications cause oral side effects. Calcium channel blockers, a common class of blood pressure medication, can cause gum overgrowth. Antihypertensives and antidepressants often cause dry mouth, removing the saliva that naturally protects teeth and gums. So the very medications keeping your heart safer can quietly make your gum disease worse.

And most people over 65 have no dental insurance. Medicare still does not cover routine dental care. This means millions of older Americans go years without a proper dental exam. Gum disease progresses undetected. By the time someone notices, significant damage has already been done.
What the Latest 2025 Research Actually Shows?
For a long time, doctors acknowledged the connection between gum disease and heart problems but weren’t sure whether treating one would help the other. That changed in 2025. In December 2025, the American Heart Association published an updated scientific statement in its flagship journal Circulation. It strengthened the 2012 position significantly.
The statement confirmed an independent association between periodontal disease and atherosclerotic cardiovascular disease, the leading cause of death globally. It also called for better communication between dental providers and heart doctors. They’ve been treating the same patients in separate silos for decades.
A 2025 Randomised Trial Changed the Conversation
The UCL team ran a proper randomised controlled trial, the gold standard in medical research. They took 135 adults with severe periodontitis and split them into two groups. One group received intensive periodontal treatment: a full mouth deep cleaning under local anaesthetic, called scaling and root planing. The other received standard care, a routine scale and polish.
Arterial Impact
Over two years, they measured carotid artery thickness as a reliable predictor of heart attack and stroke risk. The result: intensive gum treatment slowed the thickening of those arteries. It also improved endothelial function, the health of the inner lining of blood vessels.
This wasn’t just a change in inflammation markers on a blood test. It was a measurable change in arterial structure. Previous was mostly observational, which showed that gum disease and heart disease occurred together. This trial showed that treating gum disease actively reduced cardiovascular damage. That’s a meaningful step forward.
In October 2025, a separate systematic review covering 25 years of literature confirmed that chronic periodontal inflammation consistently raises CRP, interleukin 6, and TNF α, all proven cardiovascular risk markers, and that periodontal therapy reduces the systemic inflammatory burden.
To be clear about what we know and don’t know: gum disease has not been proven to directly cause heart disease. But the 2025 evidence shows it is a significant, independent risk factor and that treating it may actively reduce heart risk. More long term trials are needed. But the direction of the evidence has shifted noticeably.
Warning Signs You Should Not Ignore After 50
Most people assume bleeding gums are caused by brushing too hard. They’re not. Bleeding gums are a sign of infection. A healthy gum does not bleed. Many of these symptoms get written off as normal ageing. They’re not normal. They’re signals.
Check yourself against this list:
- Bleeding when you brush or floss: The most common early sign, and the most ignored.
- Red or swollen gums: Healthy gums are pink and firm, not puffy or dark red.
- Gum line creeping upward: Your teeth appear longer than they used to; this is gum recession.
- Persistent bad breath: Not morning breath; bad breath that doesn’t go away after brushing.
- Loose teeth or teeth that have shifted: A sign of significant bone loss underneath.
- Pain when chewing: Uncommon in early stages, serious when it appears.
- Pus between teeth and gums: Advanced infection; this needs treatment immediately.
If you have 2 or more of these signs, don’t wait for your next annual cleaning. Schedule a dental appointment within 2 weeks. This matters for heart health, too.
Each symptom on that list means active bacterial activity in your gum tissue, bacteria that may be entering your bloodstream right now. Catching this early is not just about saving your teeth. It’s about reducing a risk factor for heart attack and stroke.
5 Steps to Protect Both Your Gums and Your Heart
Here’s the good news. None of what follows requires a specialist referral, a new prescription, or an expensive procedure to get started.
1. Ask your dentist for a periodontal screening, not just a cleaning
A routine cleaning doesn’t check for gum disease. A periodontal screening measures the depth of the pockets around each tooth using a small probe.
Pocket depths above 4mm signal periodontitis even without any symptoms. Ask for this by name. Many dentists do it automatically, but many don’t unless you ask.
2. Floss every single day
The AHA released findings showing regular dental flossing may lower the risk of stroke from blood clots and irregular heartbeats. It takes 30 seconds. It removes bacteria that your toothbrush physically cannot reach. Not flossing is not neutral; it leaves a significant source of bacterial activity untouched every day.
3. If you’re diagnosed with periodontitis, get scaling and root planing without delay
This is a non surgical deep cleaning that removes bacteria from below the gum line and smooths the root surface so gums can reattach.
It’s the same treatment the UCL trial used, which measurably slowed carotid artery thickening. This is not the same as a regular cleaning. Ask specifically whether you need it.
4. Treat the risk factors you share

Quitting smoking reduces gum disease severity and cardiovascular risk at the same time. Controlling blood sugar in type 2 diabetes reduces the severity of periodontal inflammation. These aren’t separate health goals. They feed the same outcome.
5. Tell your cardiologist about your gum health, and tell your dentist about your heart condition
The AHA statement explicitly calls for better communication between dental and medical providers. If your cardiologist doesn’t know you have periodontitis, they’re missing a risk factor. If your dentist doesn’t know you’re on heart medication, they may not know your gums are at increased risk. Be the bridge between them.
Conclusion
The link between gum disease and heart health after 50 is no coincidence. It’s biology. Bacteria from infected gums enter your bloodstream. Your immune system responds with inflammation. That inflammation damages arteries. Over the years, the risk compounds, especially when you add the shared risk factors that peak in your 50s and 60s.
Schedule a full periodontal screening this month. Not at your next annual appointment. And if you know someone over 50 who hasn’t been to a dentist in years, share this with them. The oral health and heart disease connection is one of the most overlooked risk factors in medicine. It doesn’t have to be.
⚠️MEDICAL DISCLAIMER
This article is for informational purposes only. It does not replace medical advice, diagnosis, or treatment. The information covers gum disease (gingivitis and periodontitis), heart disease risk, arterial plaque, bacterial infection, scaling and root planing, flossing, dental screenings, and the impact of medications on oral health.
Individual results vary based on age, health status, and fitness level. Before changing your exercise routine, diet, or supplement use, talk to your doctor or a qualified health professional first. If you experience chest pain, dizziness, severe joint pain, or any sudden symptom during or after exercise, stop immediately and seek medical care.