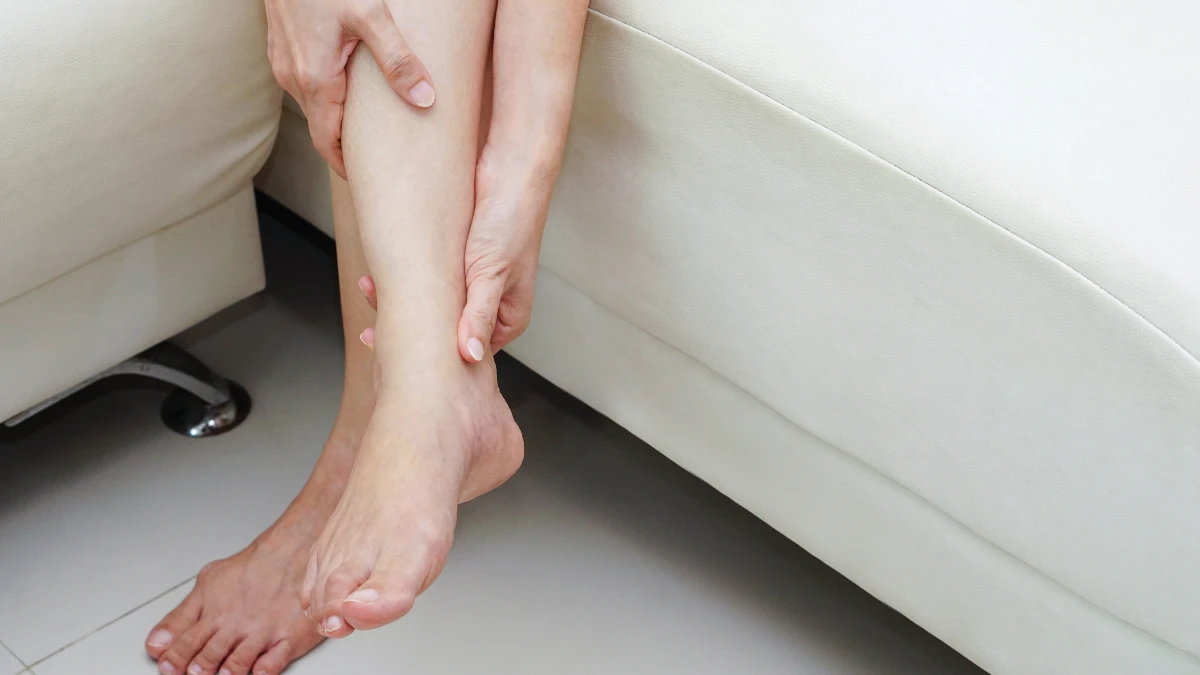
It’s 2 a.m. Your calf locks up like a fist. You stretch. You limp to the bathroom. You wait for the pain to let go. If you’re over 55, this might happen a few times a week. And you’ve probably tried everything: stretching before bed, drinking more water, buying magnesium spray off Amazon.
But here’s what most people don’t know: nighttime leg cramps are often a mineral problem. Not a stretching problem. Not a getting old problem. A mineral gap in your diet that’s easy to miss and possible to fix. Nocturnal leg cramps affect 46 56% of adults over 60, according to a 2020 study in Scientific Reports.
Up to 60% of all adults report having had them at some point American Academy of Family Physicians. And most doctors still reach for stretching advice or prescription meds. This guide covers 7 minerals that directly affect nighttime muscle cramps. You’ll learn why older adults run low on them, which foods supply them, and what you can do starting tonight.
Mineral #1 — Magnesium: The One Your Muscles Need to Relax
Here’s something most people don’t know: calcium makes your muscles contract. Magnesium makes them let go. When you’re low on magnesium, the release signal gets weaker. Your muscles stay tighter for longer. That’s where cramps come in. More than half of US adults don’t hit the recommended daily intake of 320 420 mg NIH Office of Dietary Supplements.
And as you age, your body becomes less efficient at using the magnesium you do consume. Not all magnesium supplements are the same. The forms your body absorbs best are magnesium glycinate and magnesium citrate. Magnesium oxide, the cheapest, most common form, is poorly absorbed.
A randomized, double blind clinical trial published in Nutrition Journal 2021 found that magnesium oxide monohydrate significantly reduced how often nocturnal leg cramps occurred, compared to a placebo. That’s real clinical evidence. Food sources: almonds, spinach, avocado, pumpkin seeds, dark chocolate.
Mineral #2 — Potassium: What Keeps Your Nerves and Muscles in Sync?

Your muscles don’t move on their own. They wait for a signal from your nerves. Potassium is what carries that signal and what helps stop the contraction when it’s done. When potassium gets too low, a condition called hypokalemia, muscles become weak and prone to cramping. And one of the most common causes of low potassium in older adults?
Diuretics the blood pressure medications millions of seniors take daily. Potassium doesn’t have a formal RDA the way other minerals do. It has an Adequate Intake AI instead, because research on the exact right amount is still developing. But most people aren’t getting enough regardless.
Food sources: bananas, sweet potatoes, beans, oranges, avocado, cantaloupe. If you take a diuretic, talk to your doctor about whether your potassium levels need monitoring. This is an easy blood test and is worth asking about.
Mineral #3 — Calcium: More Than Just a Bone Builder
Most people think calcium is only about bones. But calcium also fires the signal inside each muscle cell that starts a contraction. When calcium is too low, you can get muscle cramps, numbness in your fingers or toes, and even confusion. These aren’t just bone symptoms; they’re muscle and nerve symptoms.
A 2017 systematic review by van Dronkelaar and colleagues found that calcium intake is significantly tied to muscle mass in older adults. Less calcium, less muscle function. Here’s the catch: calcium can’t absorb properly without vitamin D. And many older adults are deficient in both at the same time.
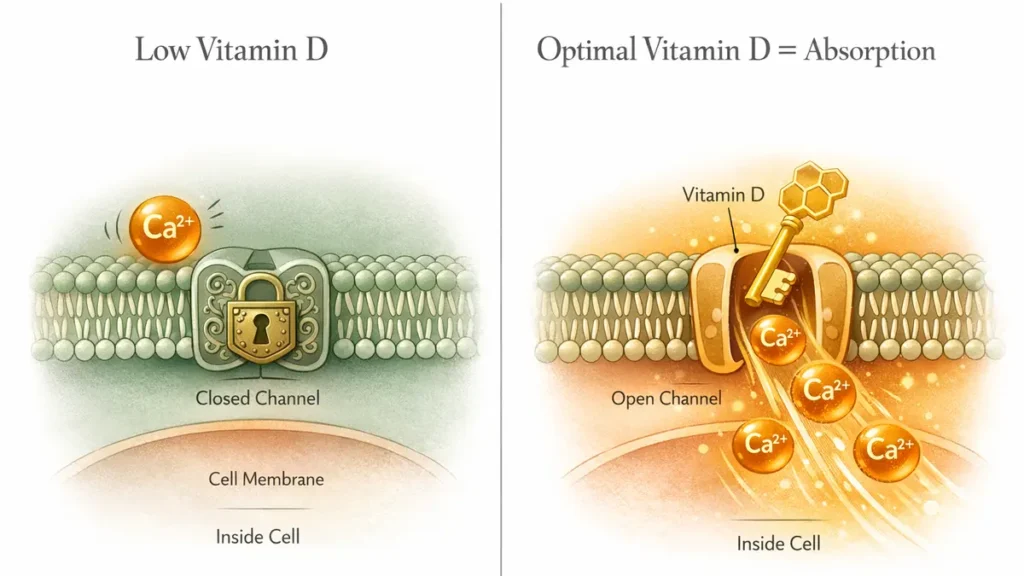
If you’re supplementing calcium and still struggling, getting your vitamin D levels tested is a smart next step. Food sources: plain yogurt, leafy greens, kale, bok choy, sardines with bones, fortified plant milks.
Mineral #4 — Sodium: The Electrolyte Seniors Are Told to Avoid

This one surprises people. Sodium gets a bad reputation because too much raises blood pressure. So many older adults cut it way back, sometimes too much. When sodium drops too low, it shifts the fluid balance around your muscle cells. That instability can trigger cramps.
Studies of athletes who cramped during events showed lower blood sodium at the finish line compared to non cramping athletes ScienceInsights.org. The same principle can apply to seniors, especially those who sweat from exercise or take diuretics. This doesn’t mean reaching for the salt shaker at every meal.
It means paying attention to balanced electrolyte intake, especially if you’re physically active or on medications that affect fluid balance. Practical tip: If you exercise, a small electrolyte drink, not just plain water, can help maintain blood volume and prevent the mineral swings that lead to cramping.
Mineral #5 — Selenium: The One Almost Nobody Talks About

Selenium probably isn’t on your radar. But it should be. A 2018 study published in the JAMDA Journal of the American Medical Directors Association by van Dronkelaar and colleagues found that serum selenium levels are significantly associated with muscle mass and physical performance in older adults. Lower selenium means weaker muscles. Weaker muscles cramp more easily.
Selenoproteins, which need selenium to function, play a direct role in how muscle cells work at the most basic level. Rederstorff et al., 2006. When you’re short on selenium, your muscle recovery suffers. The daily requirement is just 55 mcg. And here’s the wild part: one Brazil nut gives you a full day’s dose.
Other food sources: tuna, sardines, eggs, sunflower seeds, turkey. This is one of the easiest deficiencies to fix, yet almost no one talks about it in the context of leg cramps.
Mineral #6 — Zinc: What Helps Your Muscles Recover?

Zinc isn’t just for immune function. It’s needed for muscle repair. Every time you move, whether it’s a workout or just a long walk, your muscles take on microscopic stress and then repair themselves. Zinc is part of that repair process. When zinc is low, recovery slows down. Tissue stays inflamed longer. And muscles that don’t recover properly are more likely to cramp.
The same van Dronkelaar 2017 systematic review found zinc intake to be significantly linked to physical performance in older adults. The RDA is 8 mg per day for women and 11 mg for men. That sounds easy to hit, but it’s not, especially if your diet skews plant heavy without much variety.
Food sources: beef, pumpkin seeds, chickpeas, oysters, and lentils. If you eat mostly plants, you may need to be more deliberate about zinc rich choices or consider a supplement.
Mineral #7 — Phosphorus: The Fuel Your Muscles Run On
Phosphorus is involved in making ATP, the energy your muscle cells use to contract and relax. Without enough phosphorus, the basic fuel cycle of your muscles becomes less efficient. The same 2017 systematic review found phosphorus intake to be associated with sarcopenia, muscle wasting in older adults. That’s not just cramping, that’s long term muscle loss.
Here’s the irony: phosphorus is actually abundant in ultra processed foods. But that kind of phosphorus is hard to use and can actually interfere with calcium absorption, making your cramps worse, not better. The phosphorus that helps comes from whole foods.
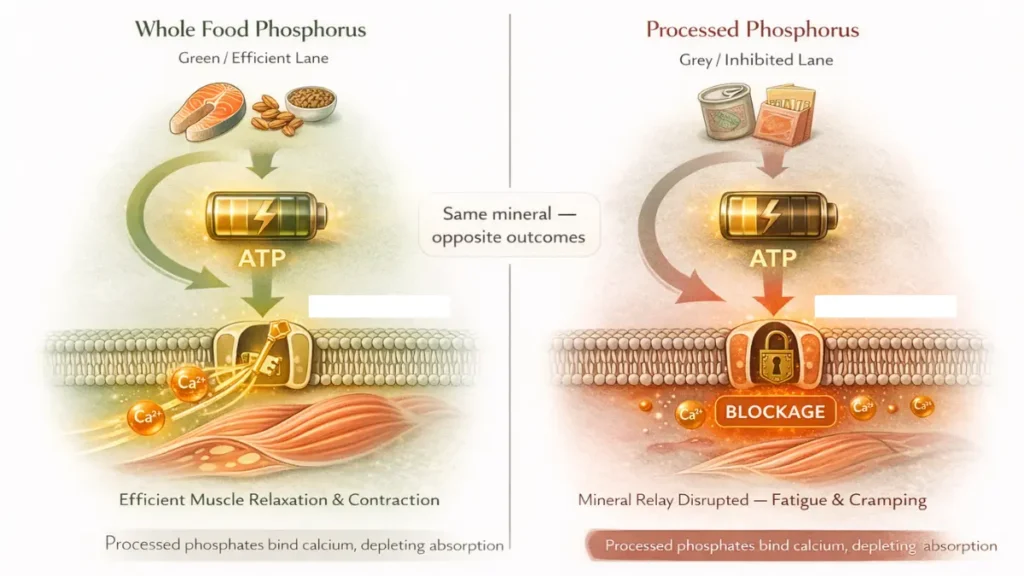
Good sources: fish, dairy, legumes, nuts, whole grains. If your diet is heavy on packaged and processed foods, switching even a few meals a week to whole food sources can shift this balance.
Conclusion
Nighttime leg cramps are common after age 55. But they’re not something you just have to live with. In most cases, the root cause is a correctable mineral gap, not an inevitable part of aging. You don’t need to take seven supplements. You need to eat more of the right foods and pay attention to a few key minerals.
Start with magnesium and potassium this week. Add selenium and zinc over the next few weeks. And if cramps keep coming back more than three nights a week, get a mineral panel done. Your muscles are telling you something. These 7 minerals for leg cramps at night are where to start listening.
⚠️MEDICAL DISCLAIMER
This article is for informational purposes only. It does not replace medical advice, diagnosis, or treatment. Before changing your exercise routine, diet, or supplement use, talk to your doctor first. If you experience chest pain, dizziness, severe joint pain, or any sudden symptom during exercise, stop and seek medical care immediately.