If you’ve ever pushed back your chair after hours of work and felt a deep, almost locked ache in your lower back as you tried to stand the problem may not be your spine.
It may be a muscle most doctors never mention. That muscle is called the psoas pronounced SO as. And it could be the reason your lower back never fully stops hurting.
Most people with chronic lower back pain try painkillers. They buy new mattresses. They do generic back stretches on YouTube. And they still wake up stiff the next morning. That’s because they’re treating the wrong thing.
The numbers show how serious this problem is. According to the Global Burden of Disease Study 2021, lower back pain affects over 619 million people worldwide.
It is the number one cause of years lived with disability on the entire planet. Yet one of the most common root causes a dysfunctional psoas barely gets talked about.
You’ll learn exactly what the psoas is, why it causes so much back pain, how to know if yours is the problem, and what you can actually do about it starting today.
What Is the Psoas Muscle? (And Why It Controls More Than You Think)
The psoas is the deepest muscle in your body. And it connects two things that should never be stuck together: your spine and your legs. Here’s a simple picture. Imagine a thick, rope like muscle buried deep inside your belly. It starts at your lower spine specifically the lumbar vertebrae L1 through L5.
It then runs down through your pelvis and attaches to the top of your thigh bone the femur. That’s the psoas. You have two of them. One on each side. It does two big jobs:
Job 1: Hip flexion. Every time you lift your knee walking up stairs, getting out of a car, kicking a ball your psoas fires. It’s the primary engine behind this movement.
Job 2: Spine stabilization. The psoas acts like a guy wire on a tent pole. It keeps your lumbar spine upright and stable. Without it working properly, your lower back has to compensate constantly. Because it attaches directly to the spine, any change in the psoas too tight, too weak, or unbalanced from side to side directly affects your posture and your pain levels.
A 2024 study published in the North American Spine Society Journal confirmed this clearly. Researchers found that the psoas is extremely important for spine stabilization and linked to clinical symptoms of patients affected by low back pain.
There’s also something most fitness articles skip. The psoas is deeply connected to your stress response.
Some researchers call it the fight or flight muscle because it physically contracts when your body feels fear or danger. Chronic stress the kind that comes from a demanding job, a packed schedule, or ongoing anxiety keeps the psoas in a state of low level contraction. Day after day.
That means even people who don’t sit all day can develop a tight, painful psoas simply from living under constant pressure. One more thing worth knowing. The psoas is so deep inside your body that you can’t directly feel it or poke it. That’s why it often gets missed.
Most pain assessments focus on the muscles you can see or touch. The psoas hides behind everything else.
The Psoas–Back Pain Connection: What Research Actually Shows
A tight or weak psoas doesn’t just cause discomfort. It physically changes the shape of your lower spine. Here’s what happens when you sit for hours at a desk, in a car, on a couch. Your psoas shortens. It stays in a bent, compressed position for so long that it starts to adapt. Over time, it forgets how to fully lengthen again. This is called adaptive shortening.
The Mechanical Tug-of-War
Functional Psoas
Neutral Alignment
Muscle is long and supple. The lumbar spine stays stacked vertically, distributing weight evenly across discs.
Shortened Psoas
Hyperlordosis
Chronic contraction pulls the vertebrae forward. This “swayback” crushes the posterior side of spinal joints.
Source: North American Spine Society Journal (2024)
Now stand up. Your shortened psoas tries to pull back but can’t. Instead, it tugs on what it’s attached to your lumbar vertebrae. This pulls your lower spine forward and down.
The result is hyperlordosis: an exaggerated curve in the lower back, sometimes called a swayback posture. Your belly tips forward. Your back arches too much.
And your spinal joints are suddenly under far more pressure than they should be. But tightness is only half the problem. A weak psoas causes just as much trouble, just differently. When the psoas is weak, it can’t stabilize your spine on its own.
The other muscles then step in your lower back muscles, your hip flexors, your quadratus lumborum.
They weren’t meant to do this job full time. They get overworked. They get strained. And you get chronic, nagging pain that never quite goes away, no matter how much you stretch your lower back. The science backs this up clearly.
Signs and Symptoms of a Tight or Injured Psoas

If your psoas is the problem, your body is already sending signals. Most people just don’t know what to look for. The most obvious sign is this: you can’t stand up straight after sitting for a while. You push up from the chair and feel an immediate, deep pull or ache in the lower back. You might even find yourself walking slightly bent forward for the first few steps.
That locked, bent over feeling? That’s often the psoas refusing to lengthen. Here are the most common symptoms of a tight or dysfunctional psoas:
Deep lower back ache. This pain usually lives at the lumbosacral junction the junction where your spine meets your pelvis. It can feel dull and constant, or sharp when you move suddenly.
Pain moving from sitting to standing. The transition is when the psoas is forced to lengthen quickly. If it can’t, it resists and that resistance is felt as pain.
Groin or hip flexor tightness. Because the psoas runs through the pelvis, a tight psoas often creates a pulling feeling in the front of the hip or deep in the groin.
Morning stiffness. The psoas shortens slightly overnight while you sleep. Standing up from bed can trigger a jolt of pain or stiffness in the lower back. Many people assume this is just how their back is. It isn’t always.
One hip sitting higher than the other. A tight psoas on one side rotates the pelvis, making one leg functionally shorter than the other. This throws off your gait and creates uneven wear across your hips, knees, and lower back.
A snapping or clicking hip. According to the NIH’s StatPearls updated May 2025, a classic sign of psoas dysfunction is a snapping sensation in the hip known as Coxa Saltans or dancer’s hip. It happens when the psoas tendon flicks over a bony point during movement. It can be painless or painful.
What Causes the Psoas to Go Wrong?
There are a handful of clear causes. And most of them are things you’re doing every single day without knowing it.
1. Sitting Too Long
This is the biggest one. When you sit, your psoas stays in a shortened, bent position. Do that for 6, 8, or 10 hours a day which is normal for office workers, remote workers, and drivers and the muscle adapts. It stops being able to lengthen fully. Physical therapist Dawn Lorring, PT, of the Cleveland Clinic put it plainly: your psoas can be aggravated from under use as well as over use.

If you’re sitting for a long period of time, your psoas muscles can get angry when you try to stand. The GBD 2021 study confirms that lower back pain is a massive burden specifically for the working age population ages 15 64, accounting for nearly 15.9 million disability adjusted life years annually. Sedentary work culture is a big reason why.
2. Overuse in Sports
Running, cycling, dancing, and sports that require repeated hip flexion all stress the psoas. So do sit ups and leg raises when done excessively. The psoas gets asked to fire repeatedly without adequate recovery time. Over time, it becomes inflamed, stiff, or develops trigger points.
3. A Weak Psoas
Not all psoas problems come from tightness. A psoas that simply isn’t strong enough fails to stabilize the spine. Other muscles pick up the slack and get overworked. This creates a locked feeling in the lower back even though the psoas itself isn’t technically tight. Stretching doesn’t fix this. Strengthening does.
4. Chronic Stress

This one surprises people. The psoas is directly wired into the fight or flight system. When your body senses threat even psychological stress the psoas contracts to prepare you to run or curl up. In short bursts, this is normal. But when stress is constant, the psoas stays partially contracted. For months. Sometimes years.
Dipalee Babaria, PT, DPT, a physical therapist at Hinge Health, explains: When we sit or stand in one position, blood flow to our muscles can decrease and cause them to feel stiff and achy Add stress induced contraction on top of that, and you have a muscle that’s fighting against you almost all day.
5. Poor Posture and Modern Life
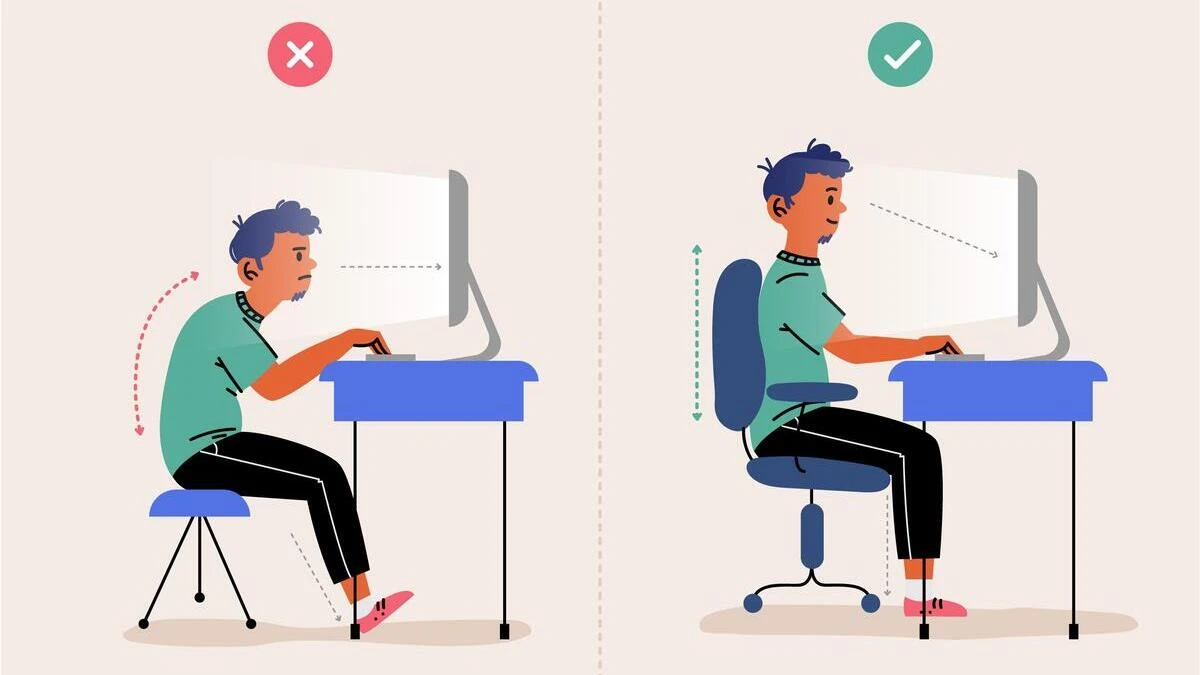
Slouching, forward head posture, and the general asymmetry of most daily activities favoring one side, crossing the same leg, always carrying a bag on one shoulder all create imbalances in how the two psoas muscles pull on the spine. None of these causes are character flaws. They’re predictable results of modern life. And they’re fixable.
When to Stop Self-Treating and See a Professional
Home exercises help most people. But some symptoms mean you need a professional, not more YouTube stretches.

See a doctor or physical therapist right away if you notice any of these:
- Numbness or tingling: in your leg, foot, or groin.
- Weakness in your leg: like your leg gives out or feels heavy.
- Pain that shoots down the back of your leg: this could be sciatica, not psoas.
- Fever combined with back pain: rare, but can signal a psoas abscess a medical emergency.
- Pain that doesn’t improve at all: after 4 6 weeks of consistent stretching and movement.
These symptoms point to conditions that look like psoas problems but aren’t or are more serious. According to StatPearls NIH, updated May 2025, less common causes of psoas syndrome include psoas abscess and retroperitoneal malignancy. These require medical evaluation, not home treatment.
Other conditions that can mimic psoas pain include:
- Disc herniation: a compressed spinal disc.
- Sciatica: nerve pain from the sciatic nerve.
- Sacroiliac joint dysfunction: pain at the back of the pelvis.
- Kidney stones: which can refer pain to the lower back.
Conclusion
The psoas is one of the most important muscles in your body. It’s also one of the most ignored. When it becomes tight from hours of sitting, stiff from chronic stress, or weak from inactivity, it pulls your lower spine out of alignment. It forces other muscles to overwork.
And it creates the kind of persistent lower back pain that painkillers, mattress upgrades, and random back stretches never fully fix. The good news is clear. With the right stretches, a few specific strengthening exercises, and something as simple as standing up every hour, most people see real improvement.
⚠️MEDICAL DISCLAIMER
This article is for informational purposes only. It does not replace medical advice, diagnosis, or treatment. Before changing your exercise routine, diet, or supplement use, talk to your doctor first. If you experience chest pain, dizziness, severe joint pain, or any sudden symptom during exercise, stop and seek medical care immediately.