You’re standing in your doctor’s office, holding a bone density result that says low. You stopped eating dairy to feel better, and now you’re worried you may have quietly made things worse for your bones. After 50, the body absorbs less calcium from food and holds onto less of it.
Most advice for adults over 50 who don’t eat dairy stops at a food list, and a food list alone will not fix this. Getting enough calcium without dairy after 50 requires a three part protocol. Each part depends on the others to work.
Part 1 — The Non-Dairy Calcium Sources Your Body Can Actually Use
Getting enough calcium without dairy after 50 starts with picking foods the body can absorb. Not all calcium sources work the same way. Kale, broccoli, sardines, firm tofu, and fortified plant milk all deliver calcium your body can use. Women over 50 need 1,200 mg of calcium per day. Men between 51 and 70 need 1,000 mg daily, and men over 70 need 1,200 mg.

The body does not absorb all the calcium in any food. How much it keeps depends on the type of food you eat. Dairy and fortified foods deliver roughly 30% of their calcium to the bloodstream. Kale and broccoli absorb at nearly the same rate, around 27%.
Canned sardines with bones provide about 325 mg of calcium per three ounces. Firm tofu made with calcium sulfate offers about 253 mg per half cup. Fortified soy or almond milk gives you 280 to 440 mg per cup. The body absorbs calcium most efficiently when amounts are under 500 mg at a time. Spreading intake across two or three meals works better than eating it all at once.
Approximately 72% of calcium in the American diet comes from dairy and dairy-containing foods. For someone who avoids dairy, that gap is real and requires a plan. Choosing the right foods is Part 1. But even the best food can be wasted if the body is not ready to absorb it.
Your Non-Dairy Calcium Shortlist
- Canned sardines with bones: about 325 mg per three ounces
- Firm tofu (calcium sulfate): about 253 mg per half cup
- Fortified soy or almond milk: 280 to 440 mg per cup
- Cooked kale: about 94 mg per cup, absorbs like milk
- Cooked broccoli: about 43 mg per cup, absorbs like milk
- White beans: about 90 mg per half cup
Aim to spread intake across meals in amounts under 500 mg at one time.
Why Spinach Is Not the Calcium Source Most People Think It Is?
Spinach has a reputation as one of the healthiest foods on earth. It is loaded with nutrients. But as a calcium source, it almost completely fails. The NIH reports that the body absorbs only about 5% of the calcium in spinach. Kale absorbs at around 27%. That is more than five times the difference from the same meal.
Spinach contains a compound called oxalic acid. Oxalic acid binds to calcium in the gut and forms a compound that the body cannot use. The calcium passes through without ever reaching the bloodstream. Swiss chard, beet greens, and rhubarb work the same way.
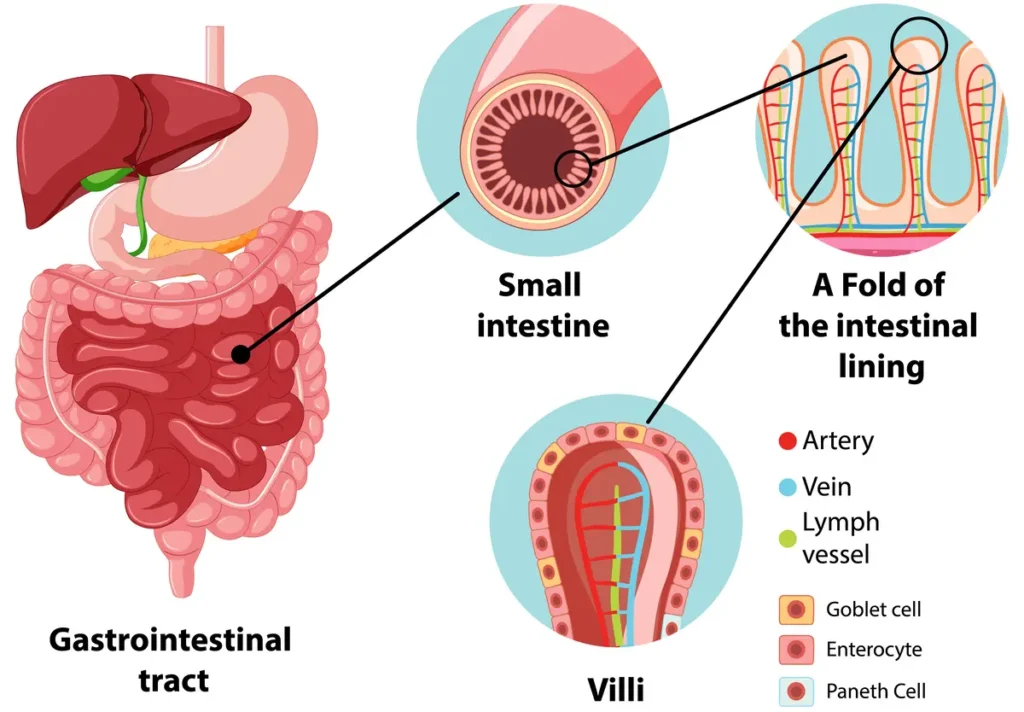
Many people over 50 who avoid dairy add spinach smoothies to their routine, believing they are protecting their bones. They are not. The calcium in that spinach is not making it through. The more carefully you add spinach to your meals for bone health, the further you may fall from your actual calcium goal, while feeling like you are doing everything right.
Knowing which foods to skip is just as important as knowing which ones to eat. And once the right foods are in place, Part 2 of the protocol determines how much of that calcium your body actually keeps.
Part 2 — The Key to How Much Calcium Your Body Keeps
Calcium does not move from food to bone on its own. It needs a signal. That signal is vitamin D. Vitamin D controls how much calcium the intestine pulls from food and sends into the bloodstream. Without enough of it, even a diet full of the right foods delivers far less calcium to the bones than it should.
If you are eating the right foods and still showing low bone density, low vitamin D is often the missing piece. A randomized trial of 76 postmenopausal women found that calcium absorption increased in a direct, measurable line as vitamin D doses rose from 800 to 4,000 IU per day.
A second study of 163 postmenopausal women with low vitamin D found that calcium absorption ranged from 52% to 58%, depending entirely on their vitamin D status. Vitamin D status determines how much of what you eat actually reaches your bones.
Vitamin D comes from sun exposure, fatty fish, egg yolks, and fortified foods. If you live in a northern climate, work indoors, or are over 60, your levels may be lower than you think. Ask your doctor to test your serum 25 hydroxyvitamin D level at your next visit. Part 2 opens the door to calcium absorption. Part 3 makes sure certain daily habits are not slamming it shut again.
Ask Your Doctor About Vitamin D
- Request a serum 25-hydroxyvitamin D test
- Optimal range: 20 to 50 ng/mL (some specialists prefer above 30)
- Food sources: salmon, sardines, egg yolks, fortified plant milk
- If deficient, a supplement is often the fastest fix
- Pair vitamin D sources with calcium-rich meals when possible
Part 3 — Three Habits That Drain Calcium Before It Reaches Your Bones
Eating the right foods and keeping vitamin D up can still fall short if certain habits quietly work against you. The first drain is high in sodium. The kidneys regulate calcium and sodium together. When sodium intake rises, calcium loss in the urine rises with it. Processed foods, canned soups, and restaurant meals are the largest sodium sources for most adults over 50.

The second drain is excess caffeine. One or two cups of coffee a day has only a small effect on calcium. Eating enough calcium throughout the day largely offsets it. Drinking four or more cups daily, especially alongside a low calcium diet, adds up over months.
The third drain is oxalic acid eaten in large quantities at the same meal as your calcium foods. You already know about spinach. The same issue applies to Swiss chard, beet greens, and rhubarb. These foods are not off limits. They simply should not be your calcium strategy. None of these drains is rare.
Most adults over 50 deal with at least one of them without knowing it. The goal is not to eliminate every risk. The goal is to know what is working against you so you can reduce it. Once you know the foods, the absorption key, and the drains, the real question becomes how all three work together as a complete system.
Why All Three Parts Must Work Together?
Part 1 is the food. Part 2 is the door. Part 3 removes what blocks it. Eat the right foods with low vitamin D, and the door is closed. Calcium comes in, but most of it passes through. Eat the right foods with strong vitamin D, but load up on high sodium meals every day, and calcium comes in and quietly leaves through the kidneys.
All three parts must run at the same time. NHANES data from 2017 to 2018 found that 43.1% of U.S. adults over 50 had low bone mass. A separate NHANES analysis found that a large share of this group fell short of calcium targets even when taking supplements.
That number does not shift with a food list alone. Timing also matters inside the protocol. Calcium carbonate supplements absorb better when taken with food. Calcium citrate works with or without food. For dietary calcium, spreading meals out keeps the intestine working at its best.
A plate that combines sardines and kale with a vitamin D source and low sodium cooking does more for your bones than any supplement taken in isolation. The problem was never a lack of food options. It was a missing framework. The three part protocol is that framework, and now it is time to put it on a plate.
Your Week 1 Action Plan
The goal this week is not perfection. The goal is to get all three parts started at the same time.

Days 1 and 2: Audit your plate. Look at what you currently eat for calcium. Write it down. Are those sources high bioavailability, like kale, broccoli, sardines, tofu, or fortified plant milk? Or are they low bioavailability, like spinach or Swiss chard? Make one swap this week. Replace spinach with kale in one meal.
Days 3 and 4: Address your vitamin D. Add one vitamin D food to your day alongside a calcium rich meal. Sardines cover both. Fortified plant milk covers both. Ask your doctor to test your serum 25 hydroxyvitamin D at your next visit.
Days 5 to 7: Find one drain. Check your sodium. Look at your caffeine. If you eat a lot of raw beans or seeds, try cooking or soaking them first. Pick one drain and reduce it this week.
Here is what a solid day looks like on this protocol. Morning: one cup of fortified soy milk gives you about 300 mg of calcium. Lunch: a sardine and kale salad delivers roughly 420 mg. Dinner: stir fried tofu with broccoli adds about 300 mg more. That is over 1,000 mg from real food, with solid bioavailability across all three meals.
Bone density changes slowly. Every week without the right inputs is a week the bones do not get what they need.
Week 1 at a Glance
Days 1 to 2: Swap one low-absorption calcium food for a high-absorption one
Days 3 to 4: Add one vitamin D source paired with a calcium-rich meal
Days 5 to 7: Find and reduce one calcium drain from your routine
Sample day: Fortified plant milk at breakfast (300 mg) + sardine-kale lunch (420 mg) + tofu-broccoli dinner (300 mg) = over 1,000 mg with high bioavailability
Conclusion
Getting enough calcium without dairy after 50 comes down to three things: the right foods, enough vitamin D to absorb them, and fewer habits that drain calcium away. Start Part 1 today. Add one high bioavailability food to your next meal, pair it with a vitamin D source, and cut one calcium drain.
⚠️MEDICAL DISCLAIMER
This article is for informational purposes only. It does not replace medical advice, diagnosis, or treatment. The information covers bone density, non dairy calcium sources, vitamin D levels, sodium intake, and caffeine intake. Individual results vary based on age, health status, and fitness level.
Before changing your exercise routine, diet, or supplement use, talk to your doctor or a qualified health professional first. If you experience chest pain, dizziness, severe joint pain, or any sudden symptom during or after exercise, stop immediately and seek medical care.