You sneeze, and it happens. You jump on the trampoline at your kid’s birthday, and it happens. You’ve been doing Kegels for six months and it’s still happening. You’re not broken. You’re just using the wrong tool. Bladder leaks affect a huge number of women over 40. Yet most women get the same advice: Do your Kegels. No explanation. No plan. Just Kegels.
The problem is that leakage after 40 isn’t just about weak muscles. Your body has changed hormones, tissue, pressure, and posture. A one size fits all fix won’t work for a body that’s gone through those changes.
Why Kegels work for some women and fail for others. What hypopressives are and what research actually says about them. How to pick the right approach based on your type of leakage. A simple 8 week plan to get started today.
Why So Many Women Leak After 40 (It’s Not Just Weakness)?
If you leak when you sneeze, your situation is different from the woman who barely makes it to the bathroom in time. And both are different from the woman who leaks during a run. The type of leak you have matters enormously. Estrogen drops, and it affects more than muscle.
When estrogen falls in perimenopause and menopause, your pelvic floor tissues lose collagen and elasticity. Kegels can build muscle. But they can’t replace lost tissue. That’s why the same Kegels that worked at 30 may not work at 48. There are three main types of leakage, and they have different causes.
Stress incontinence is when you leak during activity, such as sneezing, coughing, laughing, or jumping. Urge incontinence is when you get a sudden, powerful urge and can’t hold it. Mixed incontinence is both. After menopause, urgency and mixed types become more common, largely because of estrogen loss and changes to the bladder and urethra.
Some women are too tight, not too weak. This is called a high tone pelvic floor. If your muscles are already overactive from stress, anxiety, or years of desk work, adding more contraction Kegels makes things worse. Trying to squeeze a muscle that’s already clenched doesn’t strengthen it. It tires it out and can increase leaking.
Intra abdominal pressure is the hidden problem. Every time you cough, lift, sneeze, or run, the pressure inside your belly spikes. That pressure pushes down on your bladder. If your pelvic floor can’t handle that load, you leak. It’s not just about muscle
strength. It’s about pressure management.
The numbers are hard to ignore. Around 50% of post menopausal women have urinary symptoms. Up to 84% have some kind of genitourinary issue. And symptoms can start in your 40s; you don’t have to wait until menopause to feel them. A cohort study of over 1,600 women found that menopause was one of the strongest predictors of pelvic floor symptom severity.
What Kegels Actually Do — And When They Work?
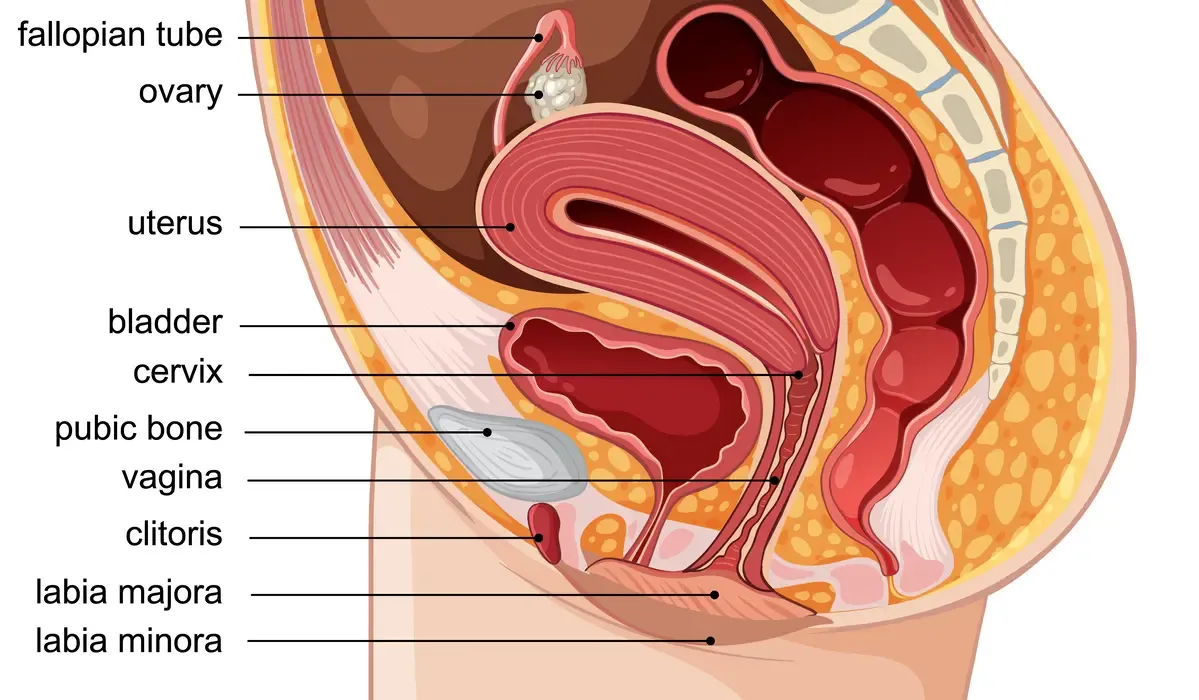
Kegels are not bad exercises. They’ve helped millions of women. Let’s be clear about that. Dr Arnold Kegel developed them to help women who leaked urine. The idea is simple: squeeze and release the pelvic floor muscles repeatedly to build strength and endurance. Specifically, you’re working the pubococcygeus and levator ani muscles, the muscles that form the base of your pelvis.
Kegels work best when:
- You have mild stress incontinence, a few drops when you sneeze or laugh.
- You’re postpartum, and your muscles are newly weakened.
- You’ve never done any pelvic floor training before.
- You can actually feel your muscles contract and release.
They recommend Kegels for women who leak a few drops while sneezing, laughing, or coughing. But they also note that Kegels are less helpful when leakage is large or when the problem is overflow incontinence. That stress incontinence responds better to Kegels than mixed incontinence.
And here’s something important that often gets left out: that Kegels only delay age related muscle loss. They don’t prevent it. The technique problem is real. Many women never learn to do Kegels correctly. Supervised Kegels with biofeedback, where a physiotherapist can confirm you’re contracting the right muscles, are significantly more effective than doing them alone at home.
And then there’s the high tone problem. If your pelvic floor is already overactive or tense, Kegels can make symptoms worse. This is more common than most women realise. Signs of high tone include pelvic pain, difficulty inserting tampons, pain during sex, or leaking that gets worse after doing Kegels.
What Are Hypopressives — And Why They Work Differently?
Forget everything you know about squeezing your pelvic floor. Hypopressives work in the opposite direction. They were developed by Dr Marcel Caufriez, a Belgian gynaecologist. He created them to help post natal women recover from pelvic floor problems.
He noticed that many traditional abdominal exercises, such as sit ups and crunches, actually increased pressure inside the belly and made pelvic floor problems worse. So he built an alternative. The core idea is pressure reduction, not contraction. Hypopressives combine specific postures, postural elongation, and a breath hold technique called expiratory apnea.
After you exhale fully, you expand your ribcage outward while holding your breath. This creates a vacuum effect inside the abdomen and thorax. That vacuum reflexively lifts the pelvic organs and activates the pelvic floor without you consciously squeezing anything.
Modern hypopressive training goes even further. It emphasises the connection between posture, breathing, and the core and pelvic floor working together as a system, not just the breath-hold trick in isolation.
What the Research Actually Shows: No Hype?

Let’s look at what studies actually found, the good and the honest caveats. The landmark 2020 RCT. Navarro Brazandez et al. assigned 94 women with pelvic floor dysfunction to one of three 8 week programs: Kegels only, hypopressives only, or both. All three groups showed significant improvements.
They reduced symptoms, improved quality of life, and increased pelvic floor muscle strength and tone both right after the program and at follow ups of 3, 6, and 12 months. The 2022 RCT. Another trial with 117 participants found that after 8 weeks of supervised hypopressive exercises.
Women had measurably improved pelvic floor muscle strength and a clear reduction in urinary incontinence severity compared to a control group who did nothing. The Katz et al. review looked at all available evidence and concluded that hypopressives do positively affect abdominal and pelvic floor muscles in women.
But the authors also said that more high quality trials are still needed. The honest nuance. Some studies found that hypopressives worked at about the same level as Kegels. A few found them slightly less effective. One study found no change in pelvic floor muscle strength after 8 weeks, but it was done in healthy women with no existing dysfunction.
Kegels vs. Hypopressives: The Side-by-Side Comparison
| Kegels | Hypopressives | |
|---|---|---|
| How they work | Active muscle contraction | Reflexive lift via pressure reduction |
| Best for | Mild stress incontinence, muscle weakness | Prolapse, urgency, high pressure, failed Kegels |
| Learning curve | Low easy to start | Moderate technique takes practice |
| Risk if done wrong | Can worsen symptoms if high-tone | Low risk; caution with hypertension |
| Time needed | Low, easy to start | 20, 30 min, 3x/week |
| Evidence base | Decades of research | Growing strong but still maturing |
| Works for menopause? | Partially | More comprehensively |
Pelvic health problems are rarely just about one muscle. Your pelvic floor doesn’t work alone. It works together with your breathing, your posture, your core, and your daily movement patterns. A practice that addresses all of those, not just the squeeze, can do more for many women over 40.

Think of it this way. Using Kegels when your real problem is intra abdominal pressure is like mopping the floor while the tap is still running. You’re cleaning up the symptom, not fixing the cause.
For women with mixed incontinence, both stress and urgency, a combined approach often makes the most sense. You get the muscle building from Kegels and the pressure management from hypopressives.
Conclusion
Kegels and hypopressives are not enemies. They’re both tools, and the right one depends on what’s actually causing your leakage. Kegels build muscle strength through contraction. Hypopressives retrain your whole pressure system from the inside out.
For many women over 40, especially those in perimenopause or post menopause, hypopressives offer something Kegels alone can’t: a way to reduce the pressure load that’s causing the problem, not just try to hold it back.
Neither works if done incorrectly. Neither works without consistency. And neither replaces a real conversation with a pelvic floor physiotherapist who can assess what’s actually going on for you.
⚠️MEDICAL DISCLAIMER
This article is for informational purposes only. It does not replace medical advice, diagnosis, or treatment. The information covers urinary incontinence, pelvic floor muscle training, hypopressive exercises, menopause, estrogen loss, pelvic organ prolapse, and intra-abdominal pressure management. Individual results vary based on age, health status, and fitness level.
Before changing your exercise routine, diet, or supplement use, talk to your doctor or a qualified health professional first. If you experience chest pain, dizziness, severe joint pain, or any sudden symptom during or after exercise, stop immediately and seek medical care.