You reach for the railing, shifting your weight tentatively as you take the first step down. There’s that familiar, sharp pinch deep in the joint, the one that makes you feel twice your actual age. You aren’t just tired; you’re starting to lose trust in your own legs.
Decades of exercise research consistently show that the lowering phase of movement builds more muscular resilience in older adults than the pushing phase alone.
If you feel your knees are already too worn out for exercise, this approach is different. Most workouts focus on the “push,” which creates high impact and grinding. This protocol focuses on the “resist,” which acts like a biological balm for your connective tissue.
It is not your fault that traditional gym advice has failed you. Most trainers ignore the very phase of movement that heals joints.
That “unsteady” feeling when you walk down stairs isn’t a permanent sentence. It’s a signal that your “brakes” are out of alignment. You can retrain those brakes starting tomorrow.
Vera winces every time she has to sit in a low armchair at her book club. She feels a dull ache that lingers long after she stands up, making her dread the walk back to her car.
Why Your “Downstairs” Strength is the Secret to Slow Lowering Knee Strength
The true protector of the knee is “eccentric” strength, the ability of your muscles to lengthen under tension. Think of your thigh muscles as the brakes on a car. If the brakes are weak, the whole vehicle shakes every time you try to slow down. When your brakes are strong, the descent is smooth and silent.
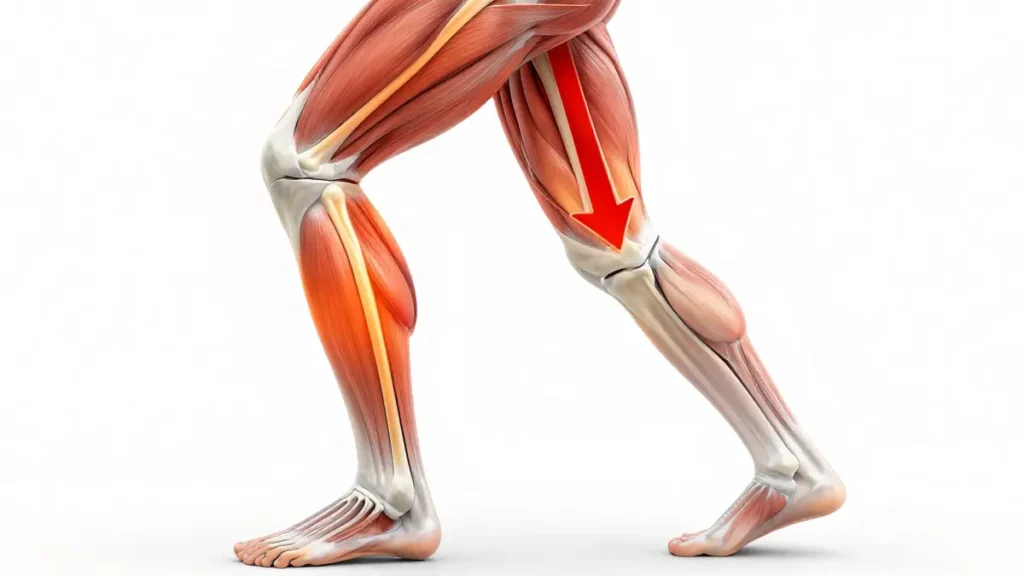
Focusing on the lowering phase allows you to bypass the “grinding” often felt during the push. Your muscles are actually stronger while lengthening than while shortening. You can handle more load with less internal joint pressure because the tension is distributed through the connective tissue rather than just the joint surface.
How to Start the Immediate Action Protocol
- Slow Seated Descents: Stand in front of a sturdy chair. Lower your hips toward the seat while counting to three. Focus on a controlled fall. Perform 5 repetitions before each meal.
- The Counter-Balanced Wall Slide: Lean against a wall with feet 12 inches away. Slide down to a shallow 45-degree angle. Hold for 2 seconds. Keep weight in your heels.
- Tier 0 Nutrition Support: Drink one cup of high-quality bone broth daily for collagen. Pair this with a vitamin C source, like a small orange, to help shuttle nutrients to the joint.
- Pain Tracking Log: Grade your knee “trust” on a scale of 1 to 10 each night. Small wins build big momentum.
The Science of Eccentric Loading: How Slowing Down Rebuilds Tissue
To fix the knee, we must stop obsessing over the joint and look at the “brakes” in the thigh. When you walk down a hill or lower yourself into a chair, your quadriceps undergo an eccentric contraction [a process where a muscle lengthens while under a load]. This specific type of tension acts as a mechanical signal to your body to repair the myotendinous junction [the interface where muscle fibers meet the tendon].
Vera notices her legs feel heavier but more stable when she focuses on the descent during her morning routine. Instead of the usual “collapse” into her sofa, she resists gravity. This resistance creates a unique type of cellular strain. While pushing a weight up builds the muscle “engine,” resisting a weight on the way down reinforces the “chassis.”

Structural Remodeling: Replacing the Frayed Bungee Cord
Your tendons are living, adaptive ropes. Years of wear can make these tissues feel like a frayed bungee cord, thin and sensitive.
Eccentric loading triggers structural remodeling, forcing the body to lay down new, organized collagen fibers. This process increases the stiffness and resilience of the connective tissue. A stiffer tendon absorbs more shock from the pavement. This means less force transfers directly into your sensitive knee cartilage.
Most people chase pain relief through rest. Rest alone doesn’t rebuild the rope.
Eccentric loading lays down new collagen in the exact direction your tendon needs to handle load. Think of it as swapping a worn-out rubber band for a steel cable, same attachment points, completely different tensile strength.
The tissue becomes more organized. The joint becomes more predictable. That predictability is what “trust” in your legs actually feels like.
Stability is a brain game. Slowing down the movement forces your brain to re-map the communication lines to your legs. Spending more time in the ‘down’ phase teaches your nervous system that the joint is safe. That grinding sound isn’t always bone-on-bone; it’s often just a lack of tension.
How to Follow the 3-Week Slow Lowering Knee Strength Protocol
Derek, a former hiker, feels skeptical that “sitting down slowly” counts as a workout. During his first attempt, he feels his thighs trembling. This trembling is his nervous system waking up. This is the part most guides skip: acknowledging that “slow” feels harder than “fast.”
Phase 1: The Foundation (Days 1–7)
- Assisted Chair Descent: Lower your hips toward a chair over a 3-second count. Use a countertop for balance.
- Seated Leg Extensions (Eccentric Focus): Straighten one leg, then slowly lower it to the floor over a 4-second count. Use your hands to help “lift” the leg back up.
Phase 2: Building Resistance (Days 8–14)
- Wall Slide Holds: Slide down a wall to a slight bend and hold for 5–10 seconds. This prepares the tendon for sustained stress.
- The Step-Down Hover: Stand on a bottom step. Hover one foot an inch above the floor for two seconds before bringing it back up.
Phase 3: Functional Integration (Days 15–21)
- Unassisted Slow Squats: Perform a squat in open space with a 5-second descent. Imagine sitting back into a deep shadow.
- The Reverse Lunge (Slow Motion): Step one foot back and slowly lower your knee. Focus entirely on the front leg resisting the descent.
How to Avoid 3 Common Mistakes That Stall Your Progress
Progress isn’t always a straight line. Recognizing “silent stalls” early keeps your momentum moving forward.
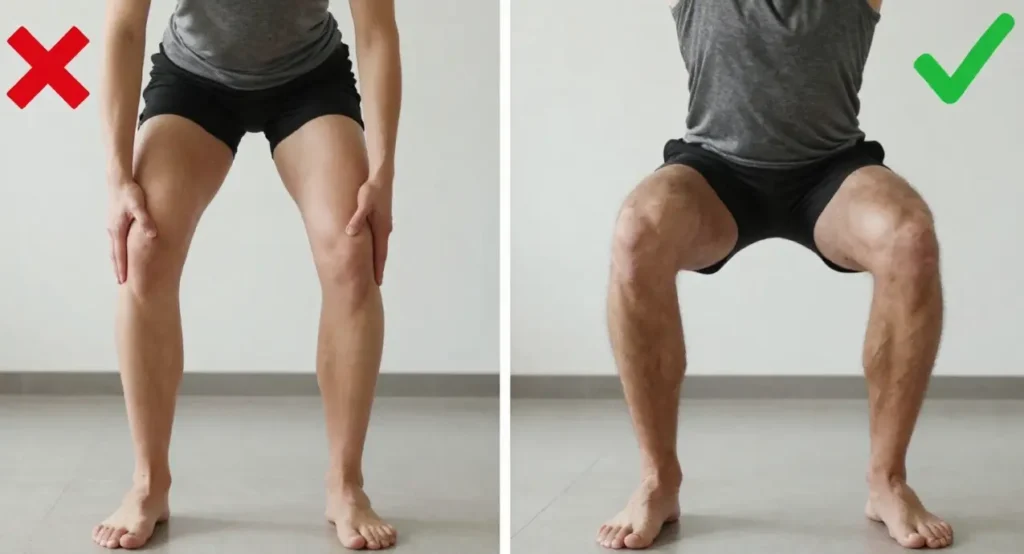
1. The “Toes-First” Weight Shift
Shifting weight onto the balls of your feet increases the shear force on the kneecap. This forces small tendons to do all the work while large muscles stay “offline.”
- The Fix: Always initiate your descent by “sitting back.” Keep your heels glued to the floor to distribute force through the entire leg.
2. Ignoring the “Valgus Collapse”
When muscles tire, knees may drift toward each other. This “caving” puts immense pressure on the inner side of the joint.
- The Fix: Watch your knees in a mirror. Your kneecap should stay in a direct line over your middle toes. If they “kiss,” reduce your depth.
3. Pushing Through “Sharp” Pain
There is a difference between a muscle burn and a joint pinch. Respect the “Stoplight Rule.”
- The Fix: Green is no pain. Yellow is a dull ache (slow down). Red is sharp pain (stop immediately). Consistency beats intensity every time.
How to Execute Your Long-Term Knee Resilience Action Plan
Derek sets a reminder on his phone to do his “slow descents” before every meal. The ritual becomes automatic. He no longer has to “think” about his knees. His body simply remembers how to engage the brakes. You are the primary investigator of your own body, and this plan is your data set.
The Weekly Maintenance Schedule
- 5-Minute Morning Reset: Perform 10 assisted wall slides and 10 slow chair descents every morning to “grease the groove.”
- Active Recovery Walks: Take 15-minute walks on flat ground. Focus on a heel-to-toe strike.
How to Support the Internal Structure with Food

- Collagen Sources: Integrate bone broth or skin-on chicken into your weekly meals.
- Vitamin C Catalysts: Include bell peppers or citrus fruits to trigger collagen synthesis.
- Hydration: Water is the primary component of synovial fluid. Think of it as the “oil” for your joints.
Progress is personal. What works in week one may shift by week three.
Your Questions Answered
Is “bone-on-bone” grinding reversible?
While you cannot regrow cartilage overnight, you can reduce the pain. Strengthening the eccentric “brakes” pulls the joint back into alignment, creating more space and reducing friction.
How soon will I feel a difference?
Most people notice a shift in “joint trust” within the first week. The neurological connection happens almost immediately, though tissue remodeling takes longer.
Can I do this if I’ve had a knee replacement?
Many people find eccentric loading helpful post-surgery, but clear it with your physical therapist first. The mechanical principles remain the same. Controlled lowering builds the stability that artificial joints often lack.
Reclaiming Your Mobility
Struggling with stairs is not an inevitable part of aging. It is a “braking” problem your body can solve. Shifting focus from the “up” to the “down” gives your knees the structural support they have been craving. You have the resources to rebuild.
Your 21-Day Checklist:
- Week 1: 3-second chair descents (3 sets of 8).
- Week 2: 10-second wall holds + Step-down hovers.
- Week 3: 5-second unassisted squats + Reverse lunges.
Vera successfully navigates the porch steps without looking for a handhold. She pauses at the bottom, surprised to realize she didn’t feel that familiar wince. The stairs are no longer an obstacle. They are just a way to get where she’s going.
⚠️MEDICAL DISCLAIMER :
This content is for informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. If you experience sharp, stabbing pain that causes your knee to “lock” or “give out,” seek professional medical care immediately.